Helpful Links:
The Fort HealthCare Comprehensive Care Management (CCM) program is founded on the belief that using an entire team to care for our patients we provide a more holistic and personalized approach that is customized to meet each patient’s healthcare needs.
About Comprehensive Care Management
It is a partnership with your primary care provider and health care team. CCM is:
- Patient-centered: A partnership between patients and their care team that allows healthcare to be individualized, empowering patients to be active participants.
- Comprehensive: A care team responsible for a patient’s physical and mental health care needs, including prevention, wellness as well as non-medical needs within acute care and chronic care.
- Coordinated: Health care is integrated across all components including pharmacy, specialty care, hospitals, home health care, community services and supports.
- Committed to quality and safety: CCM is committed to providing highly dependable care. We want to help you make informed decisions about your health by creating goals that reflect your unique health care needs.
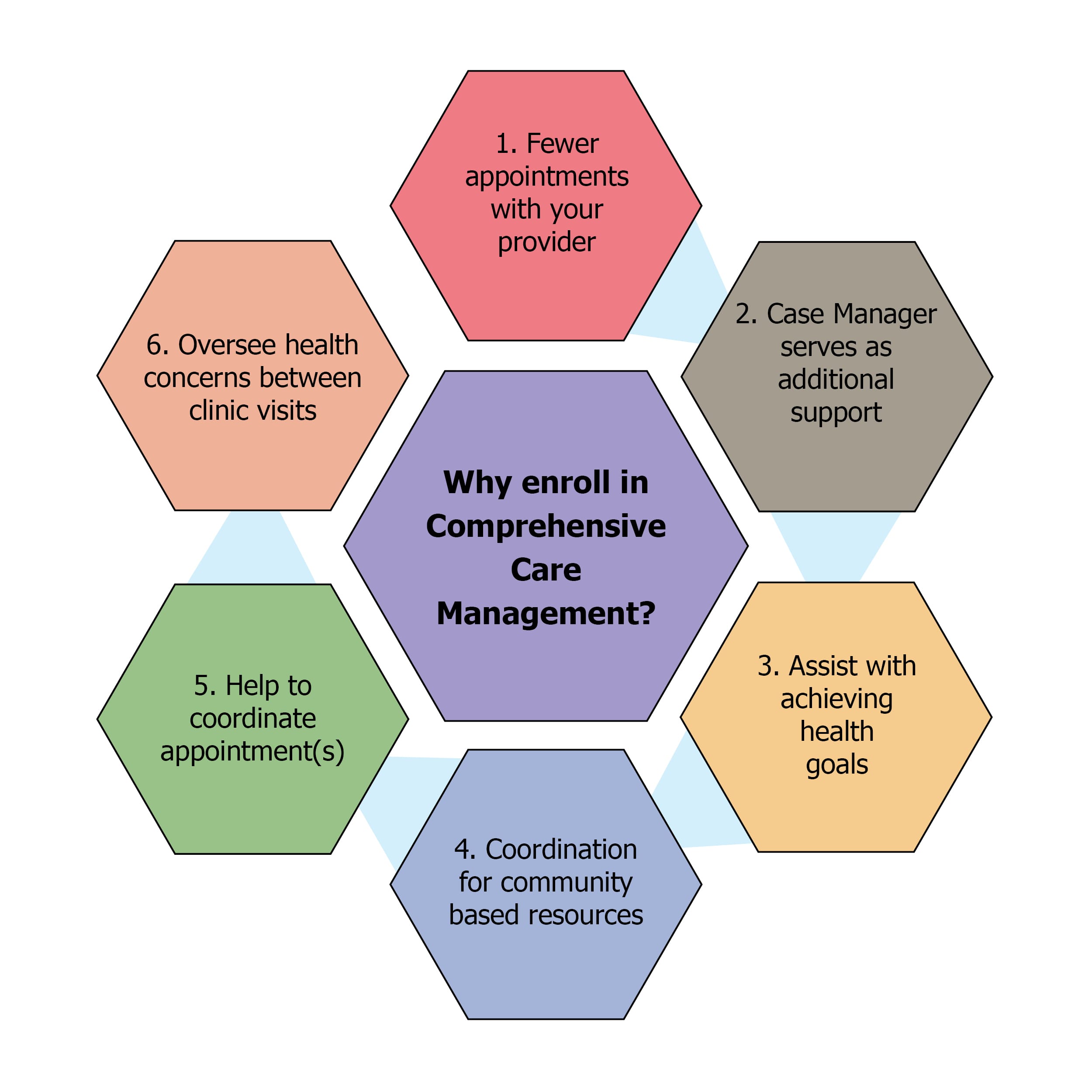
Benefits to enrolling in CCM
Nothing can replace a personal relationship with your healthcare team. Our CCM program has shown that regular interactive communication with our patients has brought about many positive changes in their lives.
Enrolled patients are finding it easier to adhere to the therapies and lifestyle changes recommended by their providers. We build personal relationships with our enrolled patients and help them bring about measurable improvements to their health.
Over the long term, our program allows patients to take charge of their health by motivating them to make achievable lifestyle changes, and educating them on skills to help relieve symptoms of their conditions.
What does an RN Case Manager do?
Your RN case manager specializes in helping you and your family manage your chronic disease. They work with you to coordinate your care, provide education regarding your illness, and help you and your primary care provider recognize when a change in treatment is needed.
Your RN case manager is here to help as much or as little as you want. They will be able to point you in the right direction so you can find information to community resources.
Once you are enrolled in the CCM program, your RN Case Manager will:
- Create a care plan that incorporates specific, short-term goals and necessary actions to achieve those goals
- Assist with finding cost effective medications
- Be your advisor and educator, helping you understand your medications, diet, activities and overall lifestyle
- Be available as a personal point of contact between you and your primary care provider in between your regularly scheduled clinic visits
How to get started with Comprehensive Care Management
Although the CCM program must be ordered by a primary care provider, anyone including family members, friends, and even the patient can contact us to request enrollment. As your health improves and you gain confidence with managing your own health care needs, case management services may no longer be necessary.
If you have any questions about Comprehensive Care Management or would like to schedule an appointment with one of our case managers, please call (920) 568-5009.
Who pays for Comprehensive Care Management?
Medicare, Medicaid, and most other insurance plans will pay for CCM Services. Though, like a physician’s office visit, you may have a deductible, co pay or out of network cost. There is no enrollment fee for CCM and financial assistance is available, if needed.
Download Brochure